Gastric volvulus is an unusual diagnosis to make in paediatric practice but is associated with significant morbidity. Volvulus derives from the latin term volvere, meaning to turn or twist.
In 1579, Ambrose Pare documented the first case of gastric strangulation. In 1866 Berti described the entity as it is known today. In 1897 Berg reported the first surgical correction of gastric volvulus with trocar decompression and reduction. In 1899 Oltman reported a 15- year-old boy who died of strangulation and necrosis of gastric volvulus. In 1904 Borchardt introduced the classical clinical triad of acute gastric distention, retching and inability to introduce a nasogastric tube1. The radiologic appearence was described by Rosselt in 19202 and the anatomic classification used today was presented by Singleton in 19403.
Since 1866 about 100 paediatric cases of this clinical entity have been described in the world literature. The sex distribution is almost equal, with a minimal predominance of males4.
The original classification of gastric volvulus was based on the axis of gastric rotation: mesenteroaxial when the rotation is along the short axis transecting the lesser and greater curvatures; organoaxial when the rotation is along the long axis extending from the hiatus of the diaphragm to the pylorus. The first type is the most common 59% and the second constitutes 29%. The remaining 12% were either of a combined type or uspecified.
The aetiology of volvulus is most commonly secondary to other disease (70%), usually a diaphragmatic defect or, rarely, adhesions acting as an apex of rotation. The primary and so-called “idiopathic type” (30%) can only occur when there is an abnormality in the form of excessive lengthening of the normal gastric attachment (gastrophrenic, gastrohepatic, gastrocolic, and gastrosplenic). This would seem more likely to occur only when congenital laxity of these attachments exists.
Some authors divide the disorder by degrees of rotation: complete (more than 180) versus incomplete (less than 180).
Volvulus can be either acute or chronic regarding to the clinical presentation and depending on the degree of rotation of the stomach and the resulting obstruction. Acute form characterized by the triad of Borchardt. Chronic type may be presented with vomiting, nausea, abdominal distension, recurrent episodes of epigastric pain, gastrooesophageal reflux, colic, crying, retarded growth, sleep problems, anxiety, anaemia, dysphagia, dyspepsia, chest pain and even repeated respiratoty intections5,6. These symptoms can appear intermittently for weeks to years. So the chronic form is probably more common, but the symptons may be subtle.
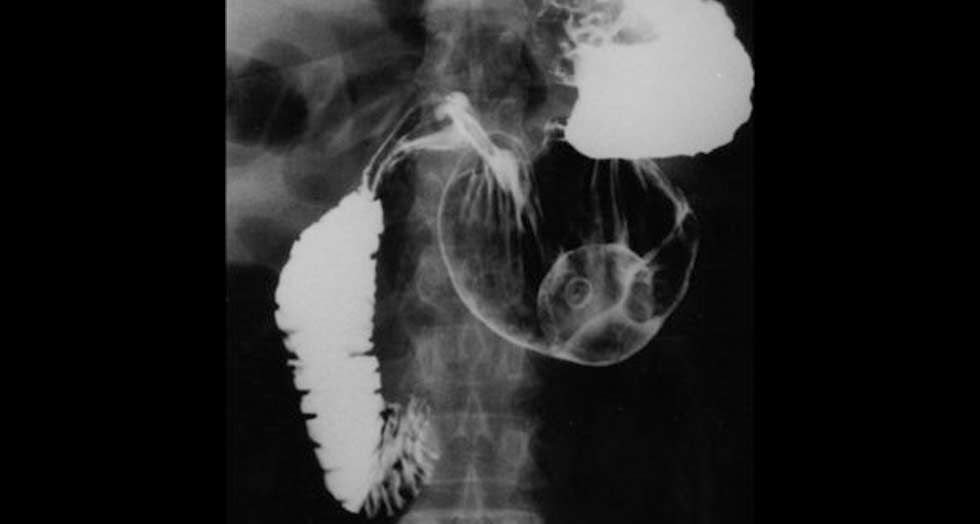
The case that we present is an organoaxial chronic gastric volvulus with non specific upper gastrointestinal symptomatology and normal plain chest , abdminal x-ray and ultrasound. This type can be difficult to recognize clinically and investigate. The most common investigations are plain-chest-abdominal radiography, endoscopy and barium study. Barium contrast studies provide the greatest yield, give a clear outline of the anatomical arragement and make the diagnosis. In our case barium meal made the diagnosis as well.
Treatment of gastric volvulus has changed in recent decades. Thirty years ago, Tanner outlined the methods of surgical repair7. These included diaphragmatic hernia repair , division of bands, simple gastropexy, gastropexy with division of the gastrocolic omentum (Tanner’s operations), patrial gastrectomy, gastrojejunostomy, fundoantral gastrogastrostomy (Opolzer’s operation) and repair of the eventration of the diaphragm. Open surgical reduction, with or without gastropexy, has been the traditional treatment. However, in recent years less invasive techniques, such as PEG placement and laparoscopic surgery, have become available. Laparoscopically fundoplication in addition to anterior gastropexy, gastropexy alone or anterolateral gastropexy have been reported with varied success8. Simple anterior gasropexy has high incidence of recurrence.
There are also reported cases with idiopathic type of gastric volvulus in which conservative treatment alone had good long-term outcome9. This modality consists of thickened feeds, small meals, and sitting in the upright position for at least 1 hour after eating.
The authors decided to treat the patient by laparoscopically anterolateral gastropexy with excellent results and uneventful recovery. We suggest that this procedure is a safe and effective treatment for idiopathic organoaxial gastric volvulus. The patient may benefit from all the advantages of a minimally invasive approach, the wound complications, quicker recovery, shorter hospitalization, decreased morbidity.
We report this case because gastric volvulus is an unusual condition that can occur in the absence of a diaphragmatic abnormality. Cureful attention to the presenting signs and symptoms and a high index of suspicion are usefull. Our experience with this patient would recommend that barium meal would be the investigation of choice in any suspected case and anterolateral gastropexy the most effective treatment.
References
- Borchardt M.(1904) Zur pathologie und therapie des magen volvulus. Arch Klin Chir 74:243-260
- Rosselet DJ.(1920) Contribution a l’etude due volvulus de estomae. J Radiol Electrol 4:341
- Singleton AC (1940) Chronic gastric volvulus. Radiology 34:53.
- Miller DL, Pasquale MD, Seneca RP (1991) Gastric volvulus in the pediatric population. Arch Surg. 126:1146-1149.
- Patel NM (1985) Chronic gastric volvulus . Report of a case and review of literature. Am J Gastroenterol 80:170-173.
- Cozat JC.Clouse RE (1998) Gastric volvulus as a cause of intermittent dysphagia. Dig Dis Sci 43:1057-1060.
- Tanner NC (1968) Chronic and recurrent volvulus of the stomach with late results of “colonic displacement”. Am Surg 115:505-15
- Bhasic DK et al (1990) Endoscopic management of chronic organoaxial volvulus of the stomach. Am J. Gastroenteral 77:1486-8
- Samaguchi S, Ohkawan H, Kemmotsu H (1981) Idiopathic gastric volvulus in infancy and childhood. 2 Kinderchir 32:218-223