Neonatal Peritonitis at the onset of Incontinentia Pigmenti.
From the clinic of Pediatric Surgery, Department of Aristotle University of Thessaloniki; School of Medicine. General Hospital ” G. Gennimatas” Thessaloniki, Greece.
Address reprint requests to Prantsoudis Euripidis specialized in the clinic of Pediatric Surgery, Depertment of Aristotle University of Thessaloniki, School of Medicine, and 40-42 Theotokopoulou P.C. 41221 Larisa, Greece. Email: eprants@yahoo.gr
ABSTRACT
Ιncontinentia pigmenti is an uncommon X-linked dominant multisystem ectodermal disorder features dermatologic, dental, ocular and central nervous system abnormalities. It is occurring in most races, but almost exclusively among females (95%). This report describes a rare case of a neonatal peritonitis in a 14 days girl who developed jejunum performation as a complication during treatment with dexamemethasone for general rash (face, trunk, limbs).In this report we discuss the clinical presentation, diagnostic evaluation, treatment options, clinical outcomes and we review the international literature
INDEX WORDS: incontinentia pigmenti disease, dexamethasone treatment, neonatal peritonitis
INTRODUCTION
Perforation of the jejunum is a rare cause of neonatal peritonitis and it is extremely rare when it presents as complication during treatment with dexamethasone. Reviewing the international literature, we found only three more cases until today.
CASE REPORT
A 14 days girl presented with a two-days history of refusal to eat, bilious vomiting and high temperature. Since the fourth day of her life she had had a rash on her trunk, face and limbs and that’s why she had taken dexamethasone drops per os. She appeared ill, disoriented and dehydrated with dry mucous membranes. She had tachycardia and tachypnea. Her abdomen was distended and tender to palpation. Bowel sounds were absent. Bilious liquid was aspirated from nasogastric tube. From serum, laboratory values had an increased number of white blood cells with neutrophilia and eosinophilia, decreased amount of potassium 3,2 mmol/lt and sodium 132 mmol/lt. She had also metabolic acidosis with arterial pH: 7,2. Abdominal radiograph slowed free intraperitoneal air (Fig.1). The newborn underwent surgical treatment. At laparotomy was found, three jejunal perforations 20 cm below the ligament of Treitz .It was performed primitive suture to prevent short bowel syndrome. Four days after laparotomy enteral content was aspirated from the abdominal drainage tube. So it was performed plain films with contrast liquid through the narogastric tube and was found the location of the leak.(fig 2) During second laparotomy was found that the leak was from the bigger one perforation of the three in the jejunum. This time a 15 cm length of small intestine was resected and intestinal continuity restored by an end-to end anastomosis. The postoperative course was uneventful. When the newborn became stable we took a skin biopsy and we found that she suffered from Incontinentia Pigmenti. At a follow-up examination 1,2 and 4 months postoperatively her growth and development has been normal. Her rash have been also improved. (fig 3,4)
DISCUSSION
It is known that the mortality rate of neonatal peritonitis is still very high in spite of the improvement of intensive care units, diagnostic methods and the level of doctor’s education. In a retrospective study of an eighty-year period the mortality rate for the patients admitted in poor condition was 95,2 % percent whereas it was 45,5 % percent for those in good conditions. Etiologically, congenital megacolon, meconium ileum and spontaneous gastrointestinal perforations were the most frequent anomalies leading to death (100%)1. The locations of gastrointestinal perforations by order of frequency are the ileum, rectosigmoid, stomach, duodenum and jejunum. The causes in order of frequency are necrotizing enterocolitis, ulcers, Hirschsprung’s disease, atresia of the small intestine, volvulus, trauma, gastroschisis, ventriculoperitoneal shunts for hydrocephalus, unknown and iatrogenic causes3. Gastrointestinal perforation can happen as complication during therapeutic or diagnostic methods or during treatment with cortisone and antiinfection drugs.
Our case is presented for its infrequency about the location of gastrointestinal perforation and its cause. Also the disease who is suffered the newborn is very rare. We reviewed the international literature and we found only on study with thee babies who developed gastrointestinal complications during treatment with Dexamethosone for chronic lung disease4.
Incontinentia pigmenti originally described by Bloch in 1992 and by Sultzberger in 1928 is also known as the Bloch-Sultzberger syndrome5. It is a rare X-Linked dominant disorder lethal in the majority of affected males in utero and variably expressed in females6. Incontinentia pigmenti affects ectodermal tissues.
Cutaneous manifestations are classically subdivided into four stages: vesicular, verrucous, hyperpigmented, and atrophic. About 80 percent of incontinentia pigmenti patients develop systematic manifestations in the form of serious complications involving the eyes, teeth, skeleton, hair, nail as well as CNS dysfuncion.
The cause of this multisystem disease is attributed to the mutations of an X-linked regulatory gene, termed nuclear factor –kappaB essential modulator ( NEMO)7,8.
Diagnosis of incontinentia pigmenti disease is made on clinical grounds, eosinophilia, biopsy and karyotype exams. Differential diagnosis must be done from herpes simplex, bullous impetigo and mastocytosis. The choice of investigative studies and the plan of management depend on the occurrence of particular noncutaneous abnormalities because the skin lesions are benign.
Therefore, the newborn that underwent treatment in our clinic combines the infrequency of incontinentia pigmenti disease and the gastrointestinal complication during treatment with dexamethasone. A high index of suspicion, careful abdominal examination, radiographic evaluation and early surgical intervention, when indicated, are critical factors influencing survival. At the time of the last clinic visit the infant was on the sixth month of her life with normal growth and development without associated anomalies and cutaneous manifestations that are classified on the third stage (fig 5).
REFERENCES
- Zorludemir U., Koca M., Olcay I., et al: Neonatal Peritonitis. Turk J Pediatr.34: 157-166, 1992
- Emanuel B., Zlotnik P., Raffensperger JG: Perforation of the gastrointestinal tract in infancy and childhood. Surg Gynecol Obstet.146:926-928, 1978
- Benz G., Roth H., Daum R: Gastrointestinal perforations in neonatal surgery. Chir Pediatr. 28:306-309, 1987
- McDonnell M., Evans N. Upper and lower gastrointestinal complications with dexamethasone despite H2 antagonist. J Paediatr Child Health. 31:152-154, 1995
- Esholdt IH: Incontinentia Pigmenti. Nord Med 109:58-60, 1994
- Berlin AL, Paller AS, Chan LS: Incontinentia Pigmenti: a review and update on the molecular basis of pathophysiology. J Am Acad Dermatol. 47:169-187, quiz 188-190, 2002
- Jean-Baptiste S, O’toole EA, Chen M, et al: Expression of eotaxin, an eosinophil-selective chemokine, parallels eosinophil accumulation in the vesiculobullous stage of Incontinentia Pigmenti. Clin Exp Immunol. 127:470-478, 2002
- Barbaro T, Falco G, Sparago A, et al: Two cases of ministerpretation of molecular results in incontinentia pigmenti, and a PCR-based method to discriminate NEMO/IKKgamma dene deletion. Hum Mutat. 21:8-11, 2003
Fig 1: Simple abdominal radiograph shows free intraperitoneal air
Fig 2: Abdominal radiograph after contrast liquid administration through nasogastric tube shows the location of leak.
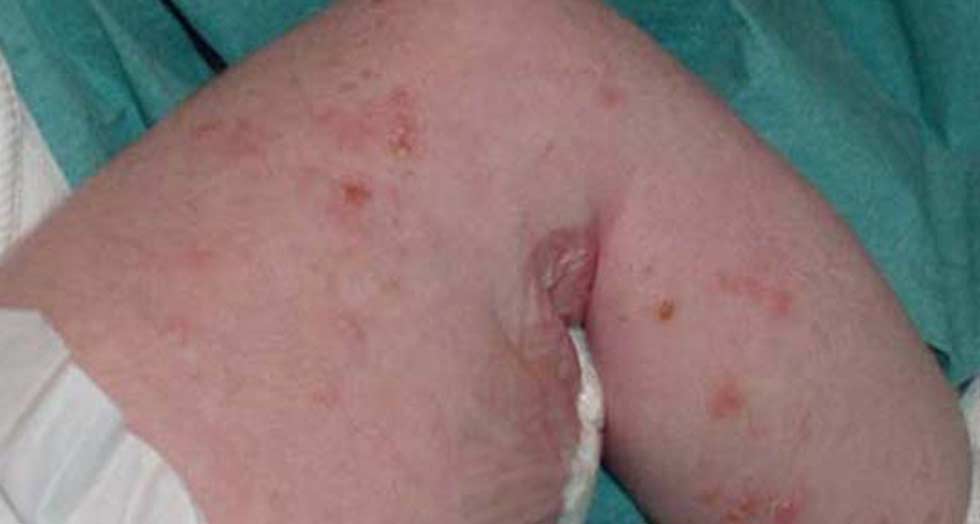
Fig 3,4: Second phase of Incontinentia Pigmenti when verrucous plaques are characteristic.
Fig 5: Epidermal hyperplasia, hyperkeratosis, and papillomatosis are characteristic on the distal limbs of our patient.